Vaginal Microbiota
The primate vagina is colonized by a vast array of microorganisms. The bulk of these microbes are bacteria, with lesser numbers of archaea and eukaryotes such as fungi. Each species' microbiome has unique components, and the organism's mating system and behavior are thought to be two of the major determinants involved in this selection. Mutualistic bacteria confer several advantages, the most notable of which is protection against pathogenic microbes. In humans, lactobacilli guard against bacterial vaginosis, yeast infections, STDs like HIV and gonorrhea, as well as a multitude of bacteria. These pathogens can affect both vitality and fecundity. Infection by streptococcus during pregnancy can lead to life threatening infections in newborns, and bacterial vaginosis can cause preterm birth. These risks are especially prevalent in the female reproductive tract, which has an increased "immunological acceptance of certain foreign cells" designed to facilitate the arrival of sperm. Thus the advantages of sacrificing nutrients to non-self cells outweighs the cost, at least while possibility of infection is high. This explains why the promiscuity of females is a major determinant of microbiome components, and why protective bacteria are not proliferative during times when individuals are not reproducing (5).
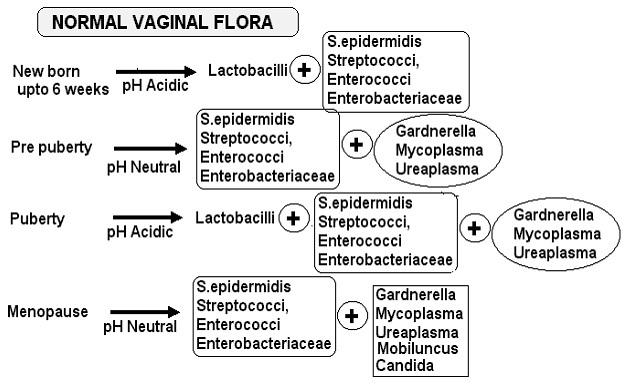
This idea is clearly demonstrated throughout the life cycle of humans, as lactobacilli are only present in large numbers after puberty and before menopause, when reproduction is likely to occur. The vaginal microbiome as a whole is chiefly controlled by estrogen. High estrogen levels result in increased glycogen stores in the vaginal wall, which is the major food source of lactobacilli. Newborns still under the influence of their mother's high estrogen levels have acidic vaginas colonized by lactobacilli, but once this estrogen leaves their system, the vaginal environment becomes neutral and the number of lactobacilli falls. The higher estrogen levels during and following puberty replenish the acidic environment and lactobacilli populations, which decline once again after menopause (5).
This idea is clearly demonstrated throughout the life cycle of humans, as lactobacilli are only present in large numbers after puberty and before menopause, when reproduction is likely to occur. The vaginal microbiome as a whole is chiefly controlled by estrogen. High estrogen levels result in increased glycogen stores in the vaginal wall, which is the major food source of lactobacilli. Newborns still under the influence of their mother's high estrogen levels have acidic vaginas colonized by lactobacilli, but once this estrogen leaves their system, the vaginal environment becomes neutral and the number of lactobacilli falls. The higher estrogen levels during and following puberty replenish the acidic environment and lactobacilli populations, which decline once again after menopause (5).
Lactobacillus
Lactobacilli are a genus of bacteria that converts glucose into lactic acid, which is necessary to keep the vagina at an ideal pH of 4.0-4.5 (6). This acid is one of the major mechanisms by which lactobacilli inhibit the growth of pathogens, in addition to the ability of some species to make hydrogen peroxide and antimicrobial peptides called bacteriocins. As well, lactobacilli fasten to the vaginal epithelium cells, preventing adherence of other microbes (7).
Disorders
Cytolytic Vaginosis
Cytolytic vaginosis, also called lactobacillus overgrowth syndrome or Doderlein's cytolysis, is caused by over-growth of Lactobacilli, which causes lysis of vaginal epithelial cells. Cytolytic vaginosis can cause itching, painful intercourse and vulvar irritation, and is often misdiagnosed as a yeast infection. Symptoms are generally most pronounced during the luteal phase of menstruation when estrogen and progesterone levels are high, and their is increased glycogen stores. It is also suggested that patients with diabetes mellitus are at higher risk for cytolytic vaginosis due to their high blood glucose levels (6).
Candidiasis
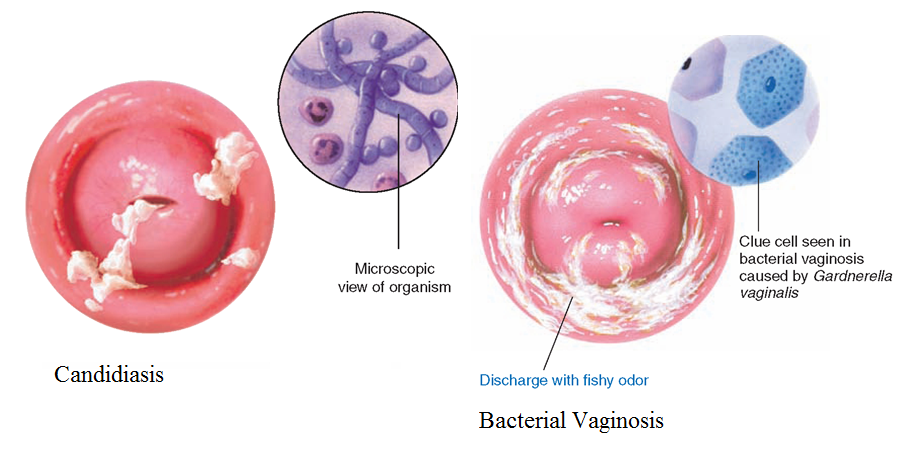
Candidiasis, also known as a yeast infection, is a common vaginal disorder caused by fungi from the Genus Candida or yeast, and has symptoms similar to cytolytic vaginosis. Yeast, like lactobacilli, feed on sugar, and are most abundant during the luteal phase of the menstrual cyle and during pregnancy when high estrogen and progesterone increase glycogen stores. Experimental results suggest that estrogen-, but not progesterone-, levels affect susceptibility to yeast infections. Researchers believe this is due to the fact that estrogen inhibits the vaginal epithelium's ability to stop Candida growth (3). This may be due to a decreased immune response during the luteal phase which is present facilitate movement of foreign sperm cells and allow successful fertilization.
Bacterial Vaginosis
Bacterial vaginosis (BV) is a disorder caused by the proliferation of bacteria other than lactobacillus in the vagina, in particular Gardnerella vaginalis. In modern times, the most common cause of BV is douching, which disturbs the balance of the vaginal microbiome by killing bacteria, including lactobacilli, allowing for colonization by pathogenic microbes. BV also causes vaginal irritation, but causes a very obvious fishy odor that distinguishes it from the other disorders (1).
Hormonal Contraceptives
Hormonal contraceptive use is very common in modern society. Many of its side-effects are common knowledge, but its effect on the vaginal microbiome is less well known. High levels of estrogen in combination contraceptives mimic the luteal phase of the menstrual cycle, increasing glycogen stores and lactobacilli numbers.
The effect of this on cases of cytolytic vaginosis have not been studied, but there is information on its impact on yeast infections and bacterial vaginosis. Hormonal contraceptive use increases the incidence of yeast infections in women, especially with the use injectable type contraceptives (2). This make sense as the naturally occurring peaks of estrogen in the body also increase a woman's chance of having a yeast infection. In BV however, hormonal contraceptive use both decreases the incidence of infections and increases it's remission. Likely, the estrogen found in these contraceptives increase glycogen stores in the vagina, bolstering lactobacilli populations, thus guarding against infection by other bacterial species (3).
Information such as this can be helpful in treating patients with these infections. It can give physicians incite into other possible contributors of yeast infections, or another treatment option for reoccurring bacterial vaginosis. Most important though, is its implications for cytolytic vaginosis. This disorder is much less studied than either yeast infections or BV, and there is no research on the effect of hormonal contraceptive use on its appearance. Yet, but applying the evolutionary theories discussed in this site, it seems that one risk factor of cytolytic vaginosis may be contraceptive use.
The effect of this on cases of cytolytic vaginosis have not been studied, but there is information on its impact on yeast infections and bacterial vaginosis. Hormonal contraceptive use increases the incidence of yeast infections in women, especially with the use injectable type contraceptives (2). This make sense as the naturally occurring peaks of estrogen in the body also increase a woman's chance of having a yeast infection. In BV however, hormonal contraceptive use both decreases the incidence of infections and increases it's remission. Likely, the estrogen found in these contraceptives increase glycogen stores in the vagina, bolstering lactobacilli populations, thus guarding against infection by other bacterial species (3).
Information such as this can be helpful in treating patients with these infections. It can give physicians incite into other possible contributors of yeast infections, or another treatment option for reoccurring bacterial vaginosis. Most important though, is its implications for cytolytic vaginosis. This disorder is much less studied than either yeast infections or BV, and there is no research on the effect of hormonal contraceptive use on its appearance. Yet, but applying the evolutionary theories discussed in this site, it seems that one risk factor of cytolytic vaginosis may be contraceptive use.
Evolutionary Significance
While the abundance and cycling female-sex hormones did not evolve as a mechanism to cultivate an advantageous vaginal microbiome, levels of estrogen have a large impact on the appearance of vaginal disease. Physiologically, estrogen modifies the vaginal environment by increasing glycogen stores, which inadvertently feed microbes. In some situations this provision is advantageous, but in others it can disrupt the delicate balance of the microbiome. By examining the relationship between the evolution of sexual development and the mutualistic relationship with lactobacilli, we can better predict which factors will have negative or positive effects on vaginal health, as well as develop a deeper understanding of less well-studied disorders.
Works Cited
1. "Bacterial Vaginosis." Wikipedia 2015. Web. 27 Apr 2015.
2. Beigi, Richard H., et al. "Vaginal Yeast Colonization in Nonpregnant Women: A Longitudinal Study." Obstetrics & Gynecology 104.5 (2004): 926-30. Web.
2. Fidel, Paul L. Jr., Jessica Cutright, and Chad Steele. "Effects of Reproductive Hormones on Experimental Vaginal Candidiasis." Infect. Immun. 68.2 (2000): 651-57. Web.
3. Riggs, Margaret, et al. "Longitudinal Association between Hormonal Contraceptives and Bacterial Vaginosis in Women of Reproductive Age." Sexually Transmitted Diseases 34.12 (2007): 954-59. Web.
4. Stumpf, Rebecca M., et al. "The Primate Vaginal Microbiome: Comparative Context and Implications for Human Health and Disease." Am. J. Phys. Anthropol. 152.57 (2013): 119-34. Web.
5. Suresh, Anupama, et al. "Cytolytic Vaginosis: A Review." Indian J Sex Transm Dis. 30.1 (2009): 48–50. Web.
6. "Vaginal Flora." Wikipedia 2015. Web. 27 Apr 2015.
Images:
Banner: https://misswalkerswiki.wikispaces.com/Lactobacillus+Acidophilus
1. http://www.tutorsglobe.com/homework-help/microbiology/anterior-urethra-72732.aspx
2. http://what-when-how.com/nursing/sexuality-fertility-and-sexually-transmitted-infections-maternal-and-newborn-nursing-part-5/
2. Beigi, Richard H., et al. "Vaginal Yeast Colonization in Nonpregnant Women: A Longitudinal Study." Obstetrics & Gynecology 104.5 (2004): 926-30. Web.
2. Fidel, Paul L. Jr., Jessica Cutright, and Chad Steele. "Effects of Reproductive Hormones on Experimental Vaginal Candidiasis." Infect. Immun. 68.2 (2000): 651-57. Web.
3. Riggs, Margaret, et al. "Longitudinal Association between Hormonal Contraceptives and Bacterial Vaginosis in Women of Reproductive Age." Sexually Transmitted Diseases 34.12 (2007): 954-59. Web.
4. Stumpf, Rebecca M., et al. "The Primate Vaginal Microbiome: Comparative Context and Implications for Human Health and Disease." Am. J. Phys. Anthropol. 152.57 (2013): 119-34. Web.
5. Suresh, Anupama, et al. "Cytolytic Vaginosis: A Review." Indian J Sex Transm Dis. 30.1 (2009): 48–50. Web.
6. "Vaginal Flora." Wikipedia 2015. Web. 27 Apr 2015.
Images:
Banner: https://misswalkerswiki.wikispaces.com/Lactobacillus+Acidophilus
1. http://www.tutorsglobe.com/homework-help/microbiology/anterior-urethra-72732.aspx
2. http://what-when-how.com/nursing/sexuality-fertility-and-sexually-transmitted-infections-maternal-and-newborn-nursing-part-5/